Technology in Oral and Maxillofacial Surgery
Alaska Center For Oral + Facial Surgery
Alaska's Only AAAHC Accredited Oral & Maxillofacial Surgery Practice

At Alaska Center For Oral + Facial Surgery, we utilize the newest and most advanced technology available for exemplary patient evaluation and treatment. We utilize a CT scanner in our office that provides excellent three-dimensional analysis for treatment planning for dental implants, corrective jaw surgery, obstructive sleep apnea surgery, and pathology or trauma treatment.
This technology also allows us to provide high-grade imaging at a fraction of the cost and radiation dose that would previously have to be done in a hospital or imaging center. When appropriate, we will also utilize our imaging system to virtually plan implant surgery, corrective jaw surgery, and correction of facial deformities. This results in more accurate surgery and shorter operation times, resulting in improved surgical outcomes and post-operative course.

Contemporary Oral and Maxillofacial Surgery At AOFS
Dr. Nordstrom’s surgical training at Legacy Emanuel Hospital was one of the three original development sites at the time for virtual surgical planning. Shortly after this development, it spread nationally and is now widely accepted. In addition to this, Dr. Nordstrom has trained and continues to operate with one of the developers of one of the most advanced protocols for surgical planning. All of this has resulted in Dr. Nordstrom having early and extensive training in the area of virtual surgical planning for the correction of facial deformities and improving the lives of his patients.
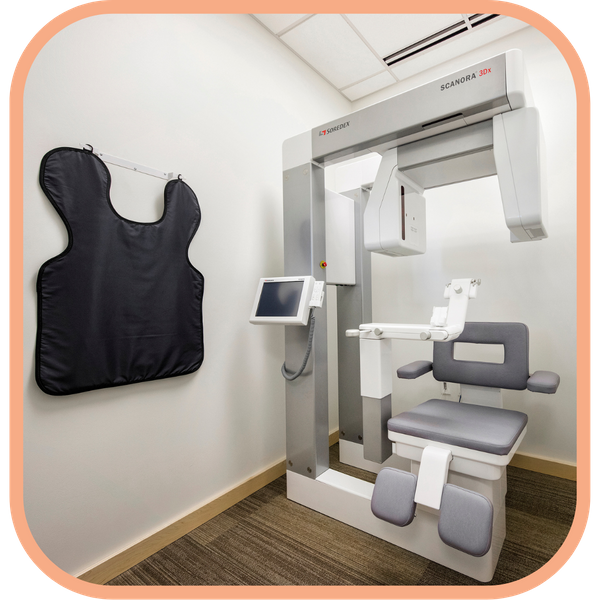
State-of-the-Art Imaging for Precision
We prioritize advanced imaging to enhance patient outcomes during oral surgery. Our in-office CT scanner provides exceptional three-dimensional imaging for accurate treatment planning. This technology allows us to conduct thorough evaluations for procedures such as maxillary advancement and the correction of dentofacial deformities. By utilizing high-grade imaging, we can minimize the costs and reduce radiation exposure when compared to traditional hospital settings. This efficient approach not only ensures the precision of our surgical plans but also streamlines the overall patient experience.
Virtual Surgical Planning for Enhanced Accuracy
Our practice harnesses the power of virtual surgical planning to elevate patient care in oral and maxillofacial surgery. By integrating sophisticated software, we meticulously plan each procedure in advance, including facial reconstruction surgery. This advanced methodology aids in simulating surgical outcomes and facilitates the effective management of complex cases. Benefits of virtual surgical planning include:
Enhanced accuracy in surgical execution
Decreased operation times
Improved post-operative recovery for patients
These innovations position us at the forefront of oral surgery, allowing us to provide the best possible care for our patients.
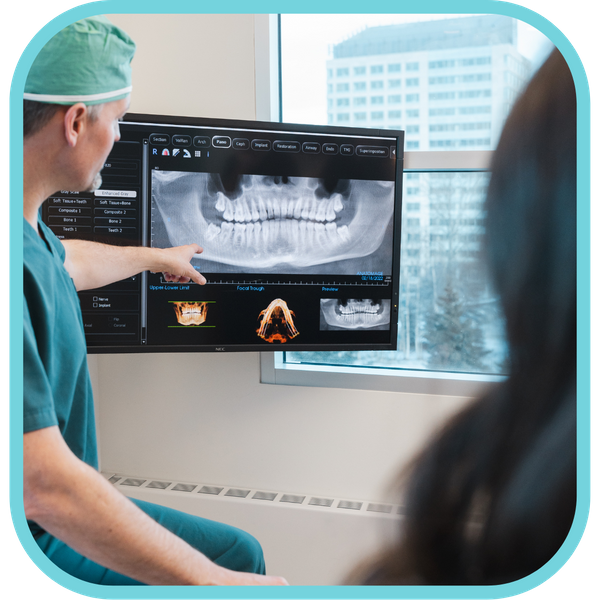
Dr. Nordstrom's Expertise in Technology
Dr. Nordstrom brings a wealth of knowledge and pioneering experience in advanced surgical technology. As one of the early adopters in this transformative field, Dr. Nordstrom continues to stay at the cutting edge by collaborating with top developers in surgical planning protocols. This expertise is instrumental not only in correcting facial deformities but also refining techniques across various procedures such as dental implants and corrective jaw surgery. Patients can trust that they are receiving care informed by the latest technological advancements and surgical methodologies.
Comprehensive Applications of Technology
Our commitment to incorporating modern technology extends to various procedures we offer at AOFS. We apply advanced imaging and surgical planning methods to a variety of conditions, ensuring comprehensive care for our patients. Some key applications include:
Dental Implants
Precise positioning for optimal integration
Corrective Jaw Surgery
Tailored planning for individual anatomical variations.
Obstructive Sleep Apnea Surgery
Customized solutions for improved airway management
Trauma Care
Swift and accurate interventions in emergency situations
By embracing these technologies, we enhance the safety and effectiveness of our surgical interventions.
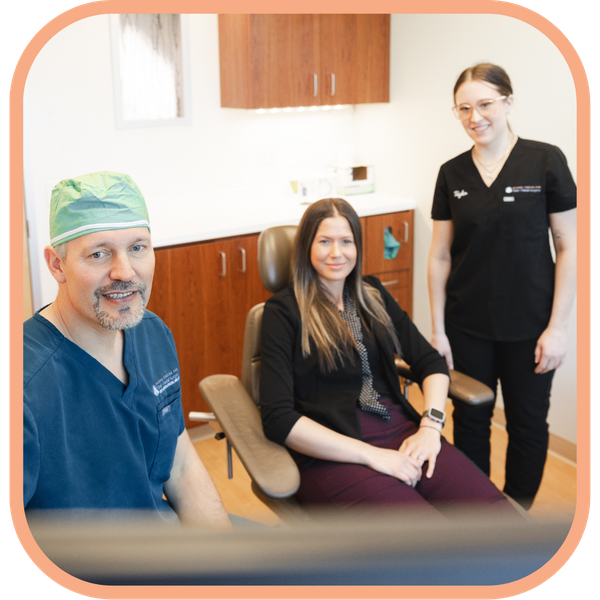
Focus on Patient-Centered Care
At AOFS, our technological advancements ultimately serve our mission of delivering compassionate, patient-centered care. We understand that oral and maxillofacial surgery can be a daunting experience, so we strive to use technology to foster confidence and comfort. Every patient receives personalized attention and detailed explanations regarding their treatment plans, ensuring that they feel informed and supported. Our state-of-the-art facility is designed not just as a center for surgical excellence, but as a welcoming space for healing and recovery.
Why Choose AOFS
Choosing Alaska Center for Oral + Facial Surgery means opting for quality care, cutting-edge technology, and an expert team dedicated to your needs. Here are several reasons why we stand out in the field of oral and maxillofacial surgery:
Highly Qualified Surgeons
Our board-certified surgeons have extensive training in both dental and medical disciplines, ensuring comprehensive care for patients of all ages.
Compassionate Care
Our entire team prioritizes comfort and satisfaction with all of our patients, fostering a supportive environment throughout your surgical journey.
Cost-Effective Solutions
With our office’s focus on high-volume efficiency, we are able to offer competitive fees without compromising on quality care or patient safety.
Discover Oral and Maxillofacial Surgery Technology
For more information on how our advanced technology can support your oral and maxillofacial surgery needs, including facial reconstruction surgery and maxillary advancement, please reach out to our office.
Alaska Center For Oral + Facial Surgery is dedicated to providing you with the care and expertise you deserve, so contact us today!
