Conditions of the Jaws, Facial Skeleton, and Skull
Alaska Center For Oral + Facial Surgery
Alaska's Only AAAHC Accredited Oral & Maxillofacial Surgery Practice

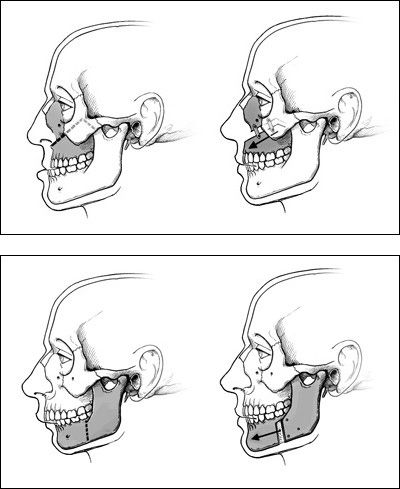
CONDITIONS OF THE JAWS, FACIAL SKELETON AND SKULL
Jaw surgery, also commonly called orthognathic surgery, is sometimes necessary to reposition the facial skeleton when orthodontic (teeth) movement alone is insufficient to achieve proper facial form and function. Corrective jaw surgery is completed to address issues including improper bite, jaw malposition or asymmetry and obstructive breathing patterns. Any of these symptoms can exist at birth, be acquired after birth as a result of hereditary or environmental influences, or as a result of trauma to the face.
Initial Consult
Initial consultation with your oral and maxillofacial surgeon will involve a thorough clinical and radiographic examination to determine indications and benefits of jaw surgery. When you are fully informed about the aspects of your care, you and your care team (most commonly including a referring dentist and orthodontist) will discuss your personalized plan and make the decision to proceed with treatment together. In preparation for your operation, your surgeon will use cutting edge computer modeling techniques to plan your surgery and show you exactly how your jaw and teeth will align after your procedure.
Surgery Day
On the day of surgery, you will receive a general anesthetic from an experienced anesthesiologist at either a local hospital or our accredited in-office surgery center. Once your jaws have been ideally positioned, they will be secured with small, biocompatible plates and screws, with no requirement to have your jaws wired shut. After you wake up from your surgery, you will be allowed to return home that day to recover in your own bed with a planned follow up in our clinic about twenty-four hours later.
Recovery
Your recovery period will commonly involve one to three weeks off from school or work, with gradual resolution of facial swelling over this time. You will be given diet instructions, which will evolve from liquid to soft chew intake for the first six weeks after surgery. At this point, you will most likely be ready to return to a regular diet and resume the final stages of your orthodontic care.
Our surgeons perform many other jaw procedures including:
- Skeletal growth problems ie: jaw size discrepancies, asymmetries, too small or too large jaws (or chin)
- Corrective jaw surgery
- Obstructive sleep apnea jaw surgery
- Tumor or cyst removal
- Bone infections
- Trauma surgery and jaw reconstruction
- Jaw joint pathology/TMJ problems
- Malocclusions or bite problems
- Cheek and/or chin implants or augmentation
Orthognathic and Reconstructive Surgery Common Terms and Definitions
- Bone – Harvesting of bone (other than Iliac Crest Bone) as appropriate for the reconstruction case in the maxillofacial environment: Using bone from a separate part of the body to add to areas of decreased bone in the jaws
- Rib grafting: Using a patient’s rib bone to repair a defect of the jaw bone
- Bone from the outer table of the calvarium: Using the outer portion of a patient’s skull to repair a defect of the jaw bone
- Bone Graft – Iliac Crest Bone Graft: Using part of the patient’s hip bone to repair a defect of the jaw bone (one of the most common sources of bone graft)
- Correction and/or reconstruction of dentofacial deformities: Correction of the position, size, shape or orientation of the jaw bone(s)
- Cranial Vault Reshaping: Surgical or orthotic (helmet) correction of the misshapen head
- Craniosynostosis Repair: Surgical correction of pediatric head deformities due to early cranial suture fusion
- Facial implants – for placement of facial/orbital prosthesis: Placement of titanium implants into the bones of the face or head in order to hold prostheses
- Distraction Osteogenesis: Making a shorter bone into a longer bone by first cutting it then slowly pulling the ends apart with a turning device and allowing new bone to fill in during the lengthening process (regularly done to increase the dimensions of the facial bones)
- Genioglossus Advancement for Sleep Apnea: Advancement of the chin and associated oral muscles in order to improve nighttime breathing
- Genioplasty (advancement, reduction, augmentation): Movement/reconstruction of the chin in order to create balance and symmetry with the rest of the face
- Implants – Related to correction or reconstruction (maxillofacial): Placement of a solid, bio-compatible material under the skin to improve facial form
- Mandibular osteotomies – total and/or segmental: The process of cutting and moving the lower jaw bone to improve facial form and function
- Maxillary/Midface segmental osteotomies: The process of cutting and moving the upper jaw bone to improve facial form and function
- Maxillomandibular Advancement for Sleep Apnea: Surgery to advance the upper and lower jaws together in order to improve nighttime breathing
- Nasal-septo-rhinoplasty associated with orthognathic surgery, facial reconstruction, or cleft surgery: Surgical repair of nasal deformity
- Primary or Secondary Bone Graft for Alveolar Cleft: Reconstruction of the hole in “gums” seen in patients with cleft lip and/or palate
- Primary or Secondary Closure of Cleft Palate and/or Alveolus: Reconstruction of the hole in the “gums” and roof of mouth seen in patients with cleft lip and/or palate
- Primary or Secondary Repair of Cleft Palate: Repair of the hole in the palate seen in patients with cleft lip and/or palate
- Primary and/or Secondary Repair of Cleft Lip: Repair of lip defects seen in patients with cleft lip
- Submucous Resection of inferior turbinates in conjunction with Orthognathic surgery: Removal of a portion of the internal nose that can cause breathing obstruction
- Septoplasty associated with orthognathic surgery, facial reconstruction, or cleft surgery: Recontouring of the “bent” internal middle portion of the nose to improve breathing
- Sleep Apnea – Maxillomandibular advancement: See maxillomandibular advancement above
- TMJ (Temporomandibular Joint): Surgical correction of painful and dysfunctional jaw joints, from minimally invasive procedures using small microscopes to custom total joint replacement
